Pharmaceutical shipments that miss their temperature window by even two hours can render entire batches unusable, costing hundreds of thousands of dollars and delaying patient care. For healthcare executives and supply chain managers operating across Southeast Asia, this is not a hypothetical risk. It is a daily operational reality. Transportation management in healthcare covers the planning, execution, and optimization of moving patients, medical supplies, pharmaceuticals, and equipment while ensuring compliance, safety, and efficiency. This guide breaks down the systems, strategies, and real-world benchmarks you need to build a transport operation that protects both margins and patients.
Table of Contents
- Understanding transportation management in healthcare
- Key systems and technologies driving efficiency
- Managing complexity: From cold chain to last-mile and patient transport
- Best practices: Strategies for optimizing transport in Southeast Asia
- Why efficient transportation is healthcare’s hidden competitive edge
- How Labgistics helps you lead in healthcare transportation
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Broad scope and impact | Healthcare transportation management covers everything from patient transfer to cold chain pharmaceuticals, directly affecting patient care and safety. |
| Modern tech advantage | Using tools like TMS, IoT, and AI enables route optimization, real-time monitoring, and compliance with regional regulations. |
| Proven strategies save costs | Regional benchmarks show that supplier consolidation and 3PL adoption can deliver 13–15% cost savings and significant capacity gains. |
| Complex barriers, actionable solutions | Managing rural access, last-mile risks, and compliance demands practical systems, local knowledge, and trusted partners. |
| Strategic investment pays off | Healthcare leaders who invest in logistical optimization gain competitive advantages for both cost and patient outcomes. |
Understanding transportation management in healthcare
With a clear introduction to why transportation management is so crucial, let’s dig into what it really encompasses in the healthcare context.
Healthcare transportation is far broader than moving boxes from a warehouse to a hospital. It spans patient, pharmaceutical, supply, and equipment movement and is especially vital for temperature-sensitive products that can degrade within hours of a cold chain breach. In Southeast Asia, where archipelagic geography and variable infrastructure add layers of complexity, the stakes are even higher.
The range of items and stakeholders involved in a single healthcare logistics network is significant:
- Temperature-sensitive pharmaceuticals, including vaccines, biologics, and oncology drugs requiring 2°C to 8°C storage
- Medical devices and equipment, which require careful handling to prevent damage and maintain sterility
- Patient transport, including non-emergency medical transport (NEMT) for scheduled procedures and inter-facility transfers
- Radioactive and controlled substances, which carry strict regulatory requirements at every handoff
- Diagnostic samples, where time sensitivity directly affects clinical accuracy
Regulatory compliance is not optional in this environment. Agencies across Southeast Asia, including Singapore’s Health Sciences Authority and Thailand’s FDA, require documented chain-of-custody records, validated transport conditions, and auditable SOPs (standard operating procedures). A single compliance failure can trigger product recalls, license suspensions, or patient harm.
Temperature control is not a logistics preference. It is a patient safety requirement. Any break in the cold chain, whether during customs clearance, last-mile delivery, or intra-hospital transfer, creates direct risk to product integrity and the patients who depend on it.
Understanding cold chain compliance in SE Asia is therefore foundational before any transportation strategy can be built. Organizations that treat compliance as a checklist rather than a core operational discipline consistently face higher error rates and regulatory exposure.
Key systems and technologies driving efficiency
After grasping the scope of healthcare transportation, let’s look at the systems and technologies making modern logistics safer and more efficient.
Modern healthcare logistics runs on a stack of interconnected platforms. TMS, IoT sensors, and real-time tracking are core for optimizing logistics and ensuring compliance, with AI-powered route optimization and automation now standard in high-performing networks. Without these tools, even well-staffed teams operate reactively rather than proactively.
A Transportation Management System (TMS) is the operational foundation. Key features to look for include:
- Real-time GPS and IoT sensor integration for live location and temperature monitoring
- Automated scheduling and carrier management to reduce manual errors and delays
- Compliance tracking modules that log every handoff, condition reading, and deviation
- Analytics dashboards that surface route inefficiencies and carrier performance trends
- API connectivity to warehouse management and hospital information systems
| TMS Feature | Adoption in Southeast Asia | Maturity Level |
|---|---|---|
| Real-time GPS tracking | Widely adopted | High |
| IoT cold chain monitoring | Growing rapidly | Medium-High |
| AI route optimization | Early adoption | Medium |
| Automated carrier management | Moderate adoption | Medium |
| Compliance audit trails | Regulatory-driven adoption | High |
AI and data analytics are changing how route decisions get made. Instead of relying on static schedules, AI systems analyze traffic patterns, weather data, customs clearance times, and historical delay data to recommend optimal routes in real time. This reduces the risk of temperature excursions during transit and cuts fuel and carrier costs simultaneously. For a deeper look at how this works in practice, AI for cold chain logistics is worth reviewing alongside your current TMS evaluation.
Pro Tip: Before selecting a TMS, confirm it can integrate with your existing hospital or laboratory management software via open APIs. A system that operates in isolation creates data silos and increases the risk of missed compliance events.
For teams managing safe pharma cold chain requirements, pairing your TMS with validated IoT sensors and medication reference tools helps staff make faster, better-informed decisions at the point of care and during transport handoffs.

Managing complexity: From cold chain to last-mile and patient transport
Understanding the technology landscape, the next challenge is managing operational complexity across different healthcare transport segments.
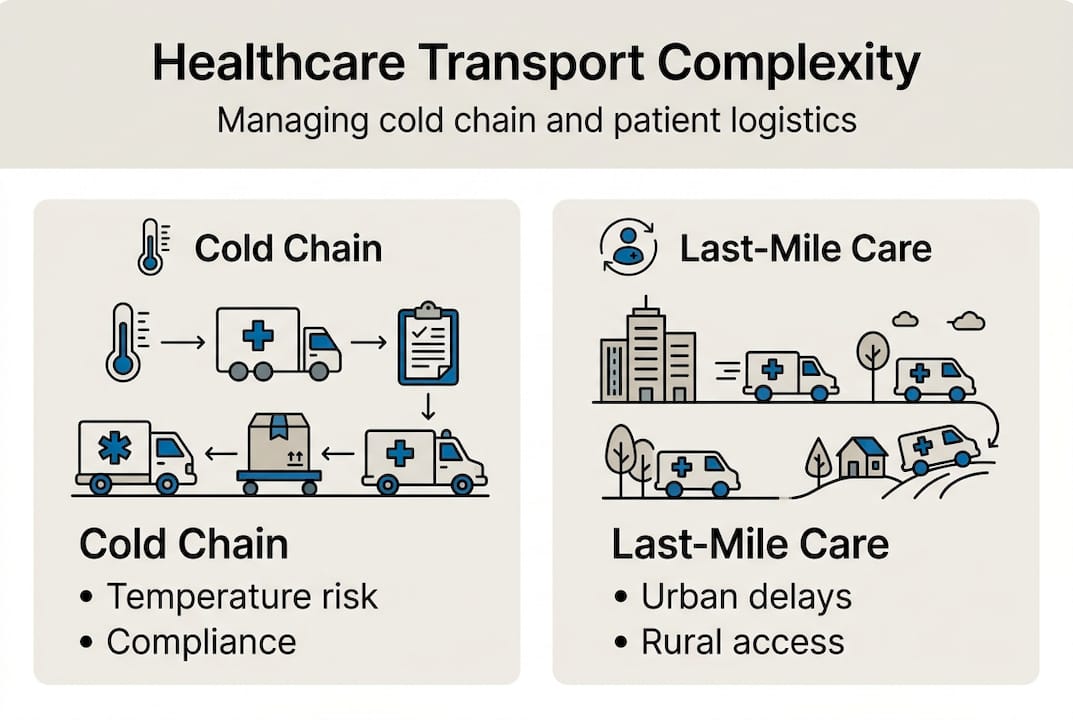
Disruptions, rural-urban disparities, temperature excursions, compliance issues, and capacity constraints affect transport effectiveness across every segment of healthcare logistics. Cold chain pharmaceutical transport and patient transport look very different operationally, but both share a zero-tolerance requirement for failure.
| Transport Type | Key Challenge | Urban Context | Rural Context |
|---|---|---|---|
| Cold chain pharma | Temperature excursions | Traffic delays, customs | Limited cold storage, poor roads |
| General medical supply | Delivery timing | High volume, congestion | Infrequent routes, low capacity |
| Patient (NEMT) | Time windows, patient safety | Scheduling density | Long distances, limited vehicles |
| Diagnostic samples | Time sensitivity | Lab proximity | Sample degradation risk |
For cold chain logistics in Southeast Asia, the rural-urban gap is particularly acute. A pharmaceutical shipment moving from Singapore to a rural clinic in Indonesia or the Philippines faces customs delays, limited refrigerated transport options, and unreliable power infrastructure. Each of these is a potential excursion point.
Minimizing last-mile risks requires a structured approach:
- Map every handoff point in the transport chain and assign a responsible party with documented accountability
- Pre-qualify carriers based on cold chain capability, compliance history, and geographic coverage
- Install continuous monitoring devices on all temperature-sensitive shipments, not just spot-check loggers
- Define escalation protocols for excursions that trigger immediate corrective action before product reaches the end point
- Conduct post-delivery audits to capture data that improves future route and carrier decisions
Benchmarks from the region are instructive. High-performing healthcare logistics networks report 99.8% on-time delivery rates for pharmaceutical air freight and 13 to 15% EBIT savings through transport consolidation. These are achievable figures, not aspirational ones, for organizations that invest in the right systems and partnerships. Understanding supply chain risks in SEA is a critical input to building resilience into your last-mile strategy. For organizations serving rural healthcare transportation needs, additional planning for extended transit times and limited infrastructure is non-negotiable.
Best practices: Strategies for optimizing transport in Southeast Asia
Given the logistical obstacles, executives need practical strategies that drive tangible outcomes in Southeast Asia.
Supplier consolidation in SEA, 3PL adoption in Thailand, and cold chain compliance have delivered double-digit savings and capacity growth for healthcare organizations that committed to structured optimization programs. The evidence is clear: fragmented transport operations cost more and perform worse.
Proven strategies for executives and supply chain managers include:
- Supplier consolidation: Reducing the number of carriers and vendors creates volume leverage, simplifies compliance oversight, and cuts administrative costs
- 3PL partnerships: Engaging a specialized third-party logistics provider gives you access to validated infrastructure, regulatory expertise, and regional networks without capital-intensive investment
- Standardization of SOPs: Uniform procedures across all transport modes reduce variability and make compliance audits faster and more predictable
- Automation of scheduling and tracking: Removing manual steps from dispatch and monitoring eliminates a major source of human error
- Ongoing compliance oversight: Regular internal and third-party audits catch process drift before it becomes a regulatory event
The 13 to 15% cost-to-serve savings from consolidation are not theoretical. Organizations in Thailand and the Philippines that shifted from multi-vendor fragmentation to consolidated 3PL models saw measurable EBIT improvement within 12 to 18 months of implementation. The key was selecting a 3PL with both regional coverage and sector-specific compliance capabilities.
Pro Tip: Schedule quarterly performance reviews with your logistics partners that include cold chain excursion rates, on-time delivery percentages, and compliance audit scores. Tracking these metrics consistently is the fastest way to identify deteriorating performance before it affects patients or regulators.
For organizations building or refining their logistics partnerships, business support key functions covers the operational and regulatory dimensions that matter most. Teams evaluating warehouse infrastructure should also review how smart 3PL warehouses are reshaping inventory management in Singapore’s healthcare supply chain.
Why efficient transportation is healthcare’s hidden competitive edge
Most healthcare organizations still classify transportation as a cost center. That framing is both inaccurate and expensive.
The data tells a different story. NEMT delivers an 11:1 ROI by reducing avoidable hospitalizations, and organizations that invest in validated transport infrastructure report 75% warehouse capacity increases alongside the 13 to 15% EBIT savings noted above. These are not marginal gains. They are structural improvements that compound over time.
Transportation is not overhead. It is the mechanism by which every other healthcare investment reaches the patient. Organizations that optimize it gain a measurable advantage in cost control, compliance, and care delivery.
In Southeast Asia, where regulatory environments are tightening and patient expectations are rising, the gap between logistics leaders and laggards is widening. Companies that have invested in TMS platforms, real-time monitoring, and skilled 3PL partnerships are capturing market share from those still relying on manual processes and fragmented vendor networks.
The opportunity is significant. How Singapore 3PL providers are positioning as regional logistics hubs illustrates what best-in-class looks like. Executives who reframe transport as a strategic asset rather than a necessary expense will find it returns value in reliability, capacity, and competitive differentiation.
How Labgistics helps you lead in healthcare transportation
Ready to put best practices into action? Here’s how Labgistics can accelerate your healthcare transportation success.
Labgistics Asia brings over 20 years of specialized experience in healthcare logistics across Southeast Asia, with proven capabilities in cold chain management, regulatory compliance, and 3PL integration. Whether you are managing temperature-sensitive pharmaceutical distribution, navigating complex cold chain compliance requirements, or building a scalable regional transport network, Labgistics offers the infrastructure and expertise to support your goals.
From fully accredited distribution centers in Singapore to end-to-end pharma and cold chain solutions across the region, Labgistics is built for the complexity of healthcare logistics. Explore our business support in healthcare logistics services to see how we can help you optimize costs, strengthen compliance, and improve patient outcomes.
Frequently asked questions
What are the biggest challenges in healthcare transportation management?
Key challenges include temperature control for pharmaceuticals, regulatory compliance across multiple jurisdictions, last-mile access in rural areas, and managing disruptions from geopolitics or disasters that affect delivery reliability and product integrity.
How does technology improve healthcare transportation management?
Technologies like TMS, IoT sensors, and AI route optimization improve efficiency and visibility. Core methodologies include real-time tracking, scheduling automation, carrier management, and compliance tracking that reduce errors and support regulatory adherence.
What is a 3PL and why is it important in Southeast Asian healthcare logistics?
A third-party logistics provider (3PL) manages warehousing, distribution, and compliance on behalf of healthcare organizations. In Southeast Asia, 3PL models have enabled hospital supply chain optimization and supplier consolidation, delivering measurable cost and capacity improvements.
How much can healthcare organizations save through transportation optimization?
Supplier consolidation benchmarks show 13 to 15% EBIT savings and up to 75% warehouse capacity increases for organizations that implement structured transport optimization programs in Southeast Asia.
Recommended
- Top inventory management tips for healthcare logistics
- Sustainable Supply Chain Practices in Medical Warehousing
- Last-Mile Healthcare Delivery in Singapore: What Makes a 3PL Ready for Clinics, Labs, and Hospitals?
- Smart 3PL Warehouses and Inventory Management | Labgistics
- Логистика на Денталното Пътуване за Имплантни Пациенти | Момани
